Long Covid and smell: How to get the treatment you need
CNN
—
It has been months since your ability to taste and smell disappeared after contracting Covid-19. You’ve tried to make an appointment with a specialist – if you could find one – only to discover waiting lists of six months or longer.
“After the pandemic started, there was this explosion of patient calls, and we couldn’t see 10% of the patients who wanted to come into the clinic,” said Dr. Justin Turner, Associate Professor of Otorhinolaryngology and Head and Neck Surgery at Vanderbilt University Medical Center in Nashville, Tennessee.
Unfortunately, this is still the case, leaving many who have not yet regained their sense of smell and taste struggling to find help, said rhinologist Dr. Zara Patel, a surgeon who focuses on treating the nose and sinuses.
“One of the big problems we recognized early in the pandemic is that almost nobody except a few specialists knew about smell loss and how to diagnose or treat it,” said Patel, professor of otolaryngology and head and neck surgery from the Stanford University School of Medicine in California.
Both Stanford and Vanderbilt have established themselves Odor Loss Treatment and Research Clinics, two of a handful in the United States.
“The saddest and most common thing I hear from patients in my clinic who have seen multiple doctors before coming to me is that they have been told, ‘There’s really nothing you can do. You just have to see if your smell comes back over time,'” Patel said.
“The sooner we begin a definitive intervention, the more likely we are to be able to bring the smell back.”
To address the issue, Patel said she gathered 50 experts to create a 600-plus-page consensus that combines verified scientific evidence and medical best practices on odor loss.
“It is the first peer-reviewed compendium of its kind on smell,” said Patel. “And it’s freely available — not just for doctors, but for patients, so everyone can read it.”
The guidelines published in the journal International Forum of Allergy & Rhinology set out an action plan for general practitioners to assess, diagnose and treat smell loss – including referral to a specialist.
Patel encourages people with smell loss to print out the clinical evaluation (see below) and take it to their doctor.
“We wrote this as a resource for patients to represent themselves — and for physicians who simply don’t have the training or expertise in this field,” Patel said. “You don’t just have to say, ‘Oh, there’s nothing you can do about that.’ They can use these and find out about the various treatment options.”
The clinical review outlines a recommended sequence for diagnosing smell loss from any cause, not just Covid-19.
medical history: A doctor should take a detailed medical history according to guidelines. These include questions about the onset, severity, and psychological impact of smell loss, as well as possible causes such as exposure to toxic chemicals, injury or surgery to the head or nose, and radiation for cancer.
Headaches, chronic sinus problems, autoimmune disorders, some medications, and vitamin or mineral deficiencies can also be associated with smell loss Cold, flu and other viral diseases like Covid-19.
Age can also play a role – we all lose some of our sense of smell as more olfactory nerves don’t regenerate. People with Parkinson’s, Alzheimer’s and multiple sclerosis often suffer from a loss of smell due to the effects of their disease on the brain.
smell test: The doctor should perform a verified smell test. However, be aware that some tests may not be sensitive enough to catch subtle nuances of smell loss, potentially leading a doctor to say there’s nothing wrong.
Some patients had this experience early in the pandemic, when about 60% of people who had the alpha and delta variants complained of a loss of smell and taste, Turner said.
“When these patients were objectively tested, that positivity rate went up a lot — about 80% or even 90% of the patients had some form of dysfunction when you actually tested them,” Turner said.
It can also work the other way around, since many people don’t notice the nuances involved in odor restoration, said Dr. Eric Holbrook, associate professor of otolaryngology and head and neck surgery at Harvard Medical School in Boston.
“There are studies that show people have trouble judging gradual changes in their sense of smell,” Holbrook said. “Tests can differ a bit, and it can be encouraging for some people to see that there has been a change.”
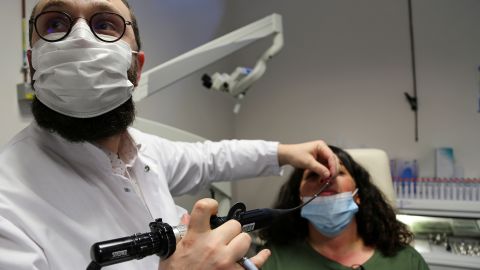
Physical work-up: A complete physical examination should be performed, including a nasal endoscopy and an examination of the cranial nerves. If the patient’s history shows evidence of a neurological disorder or chronic sinus infection, further testing should be ordered, the guidelines say.
If the tests are positive, the patient should be referred to a specialist to treat that specific disorder. For example, a person with chronic sinusitis would be referred to a rhinologist.
If a specialist is needed, Patel suggested using the American Rhinological Society website to find one near you.
The guidelines recommend different treatments depending on the cause of the loss of smell.
Underlying Disorder: If the loss of smell is due to an underlying condition, such as chronic sinusitis or a neurological condition, the guidelines suggest that doctors refer the patient to a specialist and offer treatment options.
Surgery and Trauma: If the loss is due to cranial surgery, treatment with omega-3 fatty acids is recommended. If trauma such as a car accident is the cause, oral zinc and topical vitamin A are options.
“Using the term ‘options’ means that there is either very low level data that might help,” Patel said, “or there are conflicting studies where some show it helps and some don’t, but there aren’t any Data indicative of damage. ”
viral infections: When the loss of smell is due to a viral infection such as Covid-19 or the flu, the recommended treatment is smell training, a process in which patients practice smelling scents twice a day for at least six months.
“We start with four smells that fall into different olfactory categories so that they stimulate different types of olfactory receptor neurons in your nose: lemon, rose, eucalyptus, and clove,” Patel said.
Another recommendation is to use steroids via a squeeze bottle nasal irrigator similar to a neti pot, Patel said. Steroid nasal sprays do not reach far enough up the nose to reach the olfactory nerves.
“We add a topical steroid to the salt water rinse and that allows you to bathe the neurons in the nose with a powerful anti-inflammatory drug,” she said.
Safety studies on the use of steroids in patients with chronic sinusitis have shown that the body absorbs Few steroids this way, she added, “So you don’t run into all the side effects that people get when they take steroids systemically, orally, or by injection.”
Other treatment options (not fully supported by research) for virus-induced odor loss may include topical vitamin A and omega-3 fatty oil supplements, the guidelines note.
The consensus also specifies which drugs and treatments have little to no science to support their use, such as systemic vitamin A, oral or nasal zinc, oral steroids or steroid nasal sprays, and platelet-rich plasma nasal injections.
People with loss of smell may suddenly perceive unpleasant odors: food and drink smell rotten, rotten, metallic, or chemically pungent. Doctors call the condition parosmia, which is caused when olfactory receptors fail to provide accurate information to the brain. Fake odor can occur after head injury, neurological disease or viral infections such as Covid-19.
“Parosmia is something we’ve always seen in post-viral odor loss,” Patel said, “but not nearly to the extent that we see in odor issues associated with Covid-19.”
The good news is that experts believe parosmia is a sign of recovery. The guidelines consider smell training and certain medications as treatment options.
“Some people may respond to drugs that we call neuromodulating agents — gabapentin, pregabalin, amitriptyline — drugs that modulate the nerve signal back to the brain,” Patel said.
Finally, the guidelines state that your doctor should discuss the emotional impact that a loss of smell can have and offer referrals to therapists or specialists if needed.
Some people do just fine without a sense of smell, Patel said. For others, it can lead to depression and malnutrition, especially when the smell is distorted.
“Imagine going out to eat and the food smelled and tasted like rotting meat,” Patel said. “People end up with wild swings where they lose a lot of weight, then gain a lot of weight by finding bland but very fatty or starchy foods that is safe for them.”
Groups like Fifth Sense and the Smell and Taste Association of North America have mobilized to help by offering affirmation and hope, smell training tips, and even recipes to boost appetite.
“A lot of our enjoyment of our environment actually happens through our sense of smell,” Turner said. “Simple things like the scent of spring flowers, the smell of your child and your spouse or significant other are ingrained in our minds.”